(Nejm 2004;351:2408), Flutter (Aflut) and Related Tachycardias (Including Wandering Atrial Pacemaker [WAP], Multifocal Atrial Tachycardia [MFAT] [Nejm 1990;322:1713], and Sick Sinus Syndrome [SSS])
Cause:
Associated with: higher pulse pressure widths (Jama 2007;297:709), idiopathic, CHF, rheumatic heart disease, atrial dilatation (eg, in mitral stensosis or regurgitation), pericarditis, COPD especially with hypoxia and bronchodilators, ASHD; w hyperthyroidism (Nejm 2006;354:1033; 1994;331:1252) especially in the elderly as measured by low TSH, which has a 30% 10-yr incidence in contrast to 10% 10-yr incidence w normal TSH and w toxic multinodular goiter; w alcohol intake and alcoholic myocardiopathy (Jama 2008;300:2489); w high-dose corticosteroid treatment (Ann IM 2006;166:1016)
Aflut and MFAT often (60%) from pulmonary disease including pulmonary emboli
Common; supraventricular prematures are not associated with ASHD or sudden death (Ann IM 1969;70:1159)
Sx:Polyuria, palpitations, faintness
Chronic Afib causes embolic CVA in 20% if recent CHF, HT, or previous embolus (Ann IM 1992;116:1) but <1%/yr if none of those and no increase in LA size or LV dyskinesis on echo (Ann IM 1992;116:6); likewise others find rate only 1.3% after 15 yr where no other disease and under age 60 yr (Nejm 1987;317:699); embolic CVA increased × 5 in ASHD type compared to age-matched controls, × 17 in rheumatic (Neurol 1978;28:973).
in SSS, 16% develop arterial emboli (Nejm 1976;295:190)
r/o hyperthyroidism, silent mitral stenosis, alcoholic myocardiopathy, and pulm embolism
Rx:
(Med Let 1991;33:55); all but 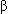 -blockers may prolong or cause ventricular arrhythmias (Ann IM 1992;117:141)
-blockers may prolong or cause ventricular arrhythmias (Ann IM 1992;117:141)
- Afib:
- Perioperative prevention post-CABG w amiodarone (Nejm 1997;337:1785)
- Rate control: iv diltiazem,
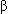 -blocker like esmolol, or digoxin but latter's rate is easily overridden by catechol/exercise stimulation (Ann IM 1991;114:573). Outcome of stroke and mortality as good or better than attempts to cardiovert (Nejm 2002;347:1825, 1834, 1883) but no estimates of morbidity outcomes like dyspnea or decr exercise capacity
-blocker like esmolol, or digoxin but latter's rate is easily overridden by catechol/exercise stimulation (Ann IM 1991;114:573). Outcome of stroke and mortality as good or better than attempts to cardiovert (Nejm 2002;347:1825, 1834, 1883) but no estimates of morbidity outcomes like dyspnea or decr exercise capacity - Conversion: especially if LA size is <50 mm, use cardioversion; embolic risk post-conversion in 1st 48 h
 1% but if >48 h is 5-7% (Ann IM 1997;126:65), but if unknown onset and TEE negative, can start warfarin × 4 wk and procede w immediate cardioversion w/o incr embolic risk (Nejm 2001;344:1411)
1% but if >48 h is 5-7% (Ann IM 1997;126:65), but if unknown onset and TEE negative, can start warfarin × 4 wk and procede w immediate cardioversion w/o incr embolic risk (Nejm 2001;344:1411) - Medical conversion w:
- Amiodarone 30 mg/kg po × 1 converts 87% (NNT = 2) (Am J Cardiol 2000;85:462; Ann IM 1992;116:1017); only safe drug to use with WPW
- Propafenone (Rythmol) 450 mg if <70 kg, 600 mg if >70 kg po, “pill in a pocket” converts 90+% w/i 1 h (Nejm 2004;351:2408), 95% w/i 6 h safely (Ann IM 1997;126:621); or
- Flecainide 200 mg po if <70 kg, 300 mg if >70 kg; or
- Ibutilide (Corvert) 1 mg iv over 10 min, repeat × 1 (Nejm 2004;351:2384); or
- Dofetilide 500 mg po bid (Med Let 2000;42:41) perhaps;
- Digoxin alone is no better than placebo (Ann IM 1987;106:503).
- Electrical cardioversion with sync and w transthoracic (AP better than ant-lateral—Lancet 2003;138:61) or esophageal-transthoracic paddles (R. Fletcher 1/00) if unstable or eventually if meds fail, ok to do even if dig on board as long as levels therapeutic and not toxic, and K+ ok (Ann IM 1981;95:676); start at 300 J not lower (Am J Cardiol 2000;86:348)
- Maintenance rx: amiodarone 200 mg po qd cheapest and best (Nejm 2007;356:935) or similar dronedarone (Nejm 2007;357:787); sotalol or other
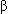 -blocker; verapamil; or digoxin, which controls resting but not exercise rate; quinidine? (Nejm 1998;338:37) po, which holds in NSR better but death rate is 3 × placebo (Circ 1990;82:1106), or procainamide; possibly dofetilide esp if in CHF (Med Let 2000;42:41; Nejm 1999;341:857, 910); or flecainide but tricky (Antiarrhythmics); class 1A drugs may increase mortality (Ann IM 2006;166:719)
-blocker; verapamil; or digoxin, which controls resting but not exercise rate; quinidine? (Nejm 1998;338:37) po, which holds in NSR better but death rate is 3 × placebo (Circ 1990;82:1106), or procainamide; possibly dofetilide esp if in CHF (Med Let 2000;42:41; Nejm 1999;341:857, 910); or flecainide but tricky (Antiarrhythmics); class 1A drugs may increase mortality (Ann IM 2006;166:719) - Anticoagulate chronic (Ann IM 2004;141:745; 1999;131:688; Jama 1999;281:182) or intermittent Afib with warfarin to INR >2 but <3.5 best balances risk and benefits (Lancet 1996;348:633, Nejm 1996;335:540, 587, 1995;333:5), which reduces risk of CVA from 7% to 1-2% at any age at least up to age 85 yr (NNT-1.5 = 25) (Circ 1991;84:527; Nejm 1990;323:1505). Annual bleeding risk ~2.5% (Ann IM 1992;116:6). But 10%/yr over age 75 yr (Jags 2005;53:655) though only 1% had fatal bleeds and doses ofen much less. Chronic AF anticoagulation benefit very small (NNT = 200) (Ann IM 1999;131:492) to nonexistent (Ann IM 1994;121:41, 54) if very low risk: age <60 yr, no h/o TIA, no valve disease, normal echo, and no hypertension. And likewise, over age 75-80 yr, risk of anticoagulation-associated intracranial bleed rises × 5, so may only be reasonable if has already had one CNS event (Neurol 2007;68:116). Use ASA if can't use warfarin (Ann IM 1999;131:492; Nejm 1990;323:1505) or pt is low risk (Jama 2001;285:2864). Warfarin to INR <2 is no better than ASA (Nejm 2003;349:1019). Addition of clopidogrel to ASA adds some protection against CVA (NNT-1=100) but at a nearly equal cost of significant bleed (Nejm 2009;360:2066, 2127) (Table 2.4)
- Catheter isolation/ablation of ectopic foci, which are often in pulmonary veins (Nejm 1998;339:659) or the left atrium. 60-80+% successful and may be 1st choice of rx (Jama 2010;303:333; Nejm 2006;354:934, 967; Jama 2005;293:2634) rarely need chronic antiarrythmics and increases EF × 20% and thus improves CHF (Nejm 2004;351:2373)
- Ablation of AV node w permanent pacer (Nejm 2001;344:1043)
- Combined atrial defibrillator/pacer devices (Nejm 2002;346:2062)
- Latrial appendage occlusion to prevent emboli? (Nejm 2009;360:2601)
- AFLUT: carotid sinus pressure trial, then rx as Afib above since >50% go on to Afib and embolic risk is as great (Ann IM 2004;140:265)
- MFAT: rx the primary disease, usually COPD or sepsis; verapamil iv with pretreatment with iv CaCl2 (Ann IM 1987;107:623) or po for chronic; Mg iv, especially if low;
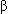 -blockers if no COPD; catheter ablation? (Circ 2002;106:649)
-blockers if no COPD; catheter ablation? (Circ 2002;106:649) - SSS: permanent pacer preferably w atrial pacing to reduce emboli (Lancet 1994;344:1523), anticoagulation, then medications to control tachycardia
Table 2.4 Treatment of Atrial Fibrillation with Antithrombotic Agents
| Risk | Treatment |
|---|
| No risk factors | Aspirin |
| 1 Moderate risk factor | Aspirin or Warfarin |
| 1 High risk factor or >1 moderate risk factor | Warfarin |
| Risk Factors |
| Moderate | High |
|---|
| 75 years or older | History of embolism, transient ischemic attack, or stroke |
| Heart failure | Mitral stenosis |
| Hypertension | Prosthetic heart valve |
Left ventricular ejection fraction  35% 35% | |
Note:Dose/INR: aspirin 81-325 mg daily; INR target 2.0-3.0.
 3 different PR intervals and P-wave morphologies; looks superficially like Afib but digoxin won't help it; WAP is same thing but rate <100
3 different PR intervals and P-wave morphologies; looks superficially like Afib but digoxin won't help it; WAP is same thing but rate <100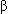 -blockers may prolong or cause ventricular arrhythmias (Ann IM 1992;117:141)
-blockers may prolong or cause ventricular arrhythmias (Ann IM 1992;117:141) 1% but if >48 h is 5-7% (Ann IM 1997;126:65), but if unknown onset and TEE negative, can start
1% but if >48 h is 5-7% (Ann IM 1997;126:65), but if unknown onset and TEE negative, can start