AUTHOR: Lydia Sharp, MD
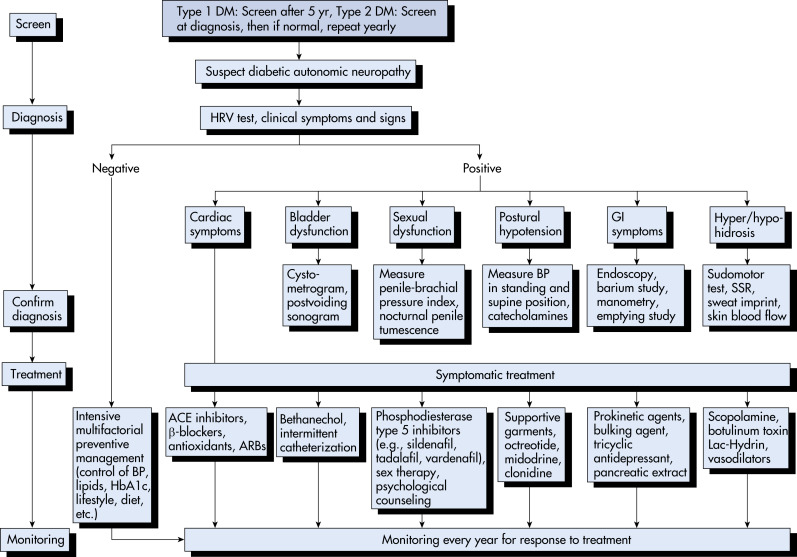
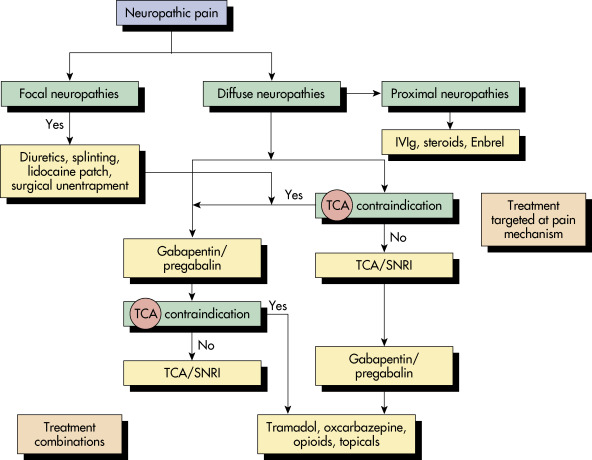
Diabetic polyneuropathy is a distal symmetric polyneuropathy (DSPN) characterized by numbness, tingling, pain, or weakness that affects the nerves in a stocking-and-glove pattern, beginning in the distal extremities. DSPN leads to substantial pain, morbidity, and impaired quality of life. A number of different classification schemes exist for diabetic neuropathy; a common one is outlined in Box 1.
Distal symmetric polyneuropathy
Diabetic peripheral neuropathy
| ||||||||||||||||||||||||||||
The prevalence of diabetic polyneuropathy varies from approximately 5% to 100% in patients with diabetes mellitus in population-based studies. It is the most common form of peripheral neuropathy in the Western world.1
Patients with poor glycemic control; other features of metabolic syndrome, such as hypertension, hypertriglyceridemia, and obesity; diabetic nephropathy; or retinopathy are at increased risk.1
- Patients most commonly experience numbness and tingling, but they may also experience either feelings of tightness or a sensation of heat or cold.2
- Pain is common, is often worst at night, and can be burning, aching, shooting, or lancinating in nature.2
- Sensory symptoms begin in the feet and may slowly ascend over months to years. Symptoms in the hands do not generally occur until symptoms in the lower extremities have reached the level of the knees. In more severe cases, the symptoms can spread to the trunk and head.2
- Neurologic examination reveals early loss of small-fiber modalities resulting in decreased pinprick and temperature sensation and later involvement of large-fiber modalities leading to a reduction in vibratory and proprioceptive sensation. Ankle reflexes are usually reduced or absent, and more proximal reflexes may also become involved as the neuropathy progresses. Strength is usually normal, but there can be some motor involvement leading to mild weakness and atrophy, which is usually limited to intrinsic foot muscles and ankle dorsiflexors.