Any lumps or lesions (location, size) or swelling in breasts? Change in size or firmness? Redness, warmth, or dimpling of breasts? Tenderness? Pain? Timing in menstrual cycle? Change in position of nipple or nipple discharge? Amount and character of discharge? Age of first menstruation? Age of client when they gave birth to children (if applicable)? Previous breast surgeries? History of breast cancer in family? Self-care: breast self-examination (BSE; frequency and time performed)? Taking any hormones, contraceptives, or antipsychotic agents, sedatives, opioid medications or medicines for high blood pressure, herbal supplements? Exposure to radiation, benzene, or asbestos? Amount of coffee, tea, or cola (or other forms of caffeine) consumed each day? Milk intake: amount, how often, and over how many years? Diet and daily exercise routine? Last breast examination? Last mammogram?
Risk for breast cancer related to increasing age, personal history of breast cancer, family history of breast cancer, early menarche and late menopause, no natural children, first child after age 30 years, no history of breastfeeding, excessive weight (especially weight gain as an adult), higher education and socioeconomic status, regular alcohol intake (2-5 drinks daily), previous breast irradiation, hormone replacement with progesterone, no or poor BSE, poor screening, lack of adequate physical activity (45-60 minutes at least 5 days/week).
Use the risk tool available at http://www.cancer.gov/bcrisktool/ to calculate client’s level of risk for developing breast cancer.
BSE guide to give to client (see Box 16-1)
Gloves and slide for specimen if nipple discharge is present
Review Figures 16-1 to 16-4 for anatomy of the breasts and regional lymphatics.
Keep in mind that the breast examination may evoke fear, anxiety, or embarrassment that may influence the client’s ability to discuss the condition of the breasts and BSE. Men with gynecomastia may be embarrassed to have what they consider a "female condition." Explain the steps and purpose of the examination. Warm your hands. Remember it is important to carefully perform the breast examination on male as well as female clients.
| ASSESSMENT PROCEDURE | NORMAL FINDINGS | ABNORMAL FINDINGS |
|---|---|---|
| Inspection | ||
| Inspect the breasts with the client in a sitting position with arms at sides, arms overhead, hands pressed on hips, palms pressed together, and arms extended straight ahead as client leans forward (Fig. 16-5). Also inspect the areolae and nipples. | ||
| Observe breasts for the following: | ||
| ||
| Observe areolae and nipples for the following: | ||
| PALPATION | ||
| Use the flat pads of three fingers to compress tissue against breast wall gently. Palpate with client sitting. Then have client lie down and place arm of side being examined overhead with small pillow under upper back. Palpate in circular motion starting at the 12-o’clock position and moving in concentric rings inward to areola and nipple (Fig. 16-6A). Bimanual palpation may be used in large-breasted clients. A wedge (Fig. 16-6B) or vertical (Fig. 16-6C) pattern may be used if preferred. | ||
| Palpate breasts for the following. | ||
|
| |
| Palpate nipple gently for discharge (Fig. 16-7). | ||
| ||
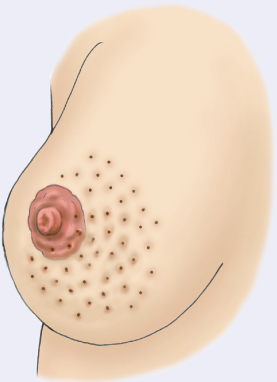
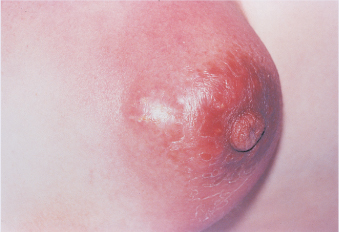
Resulting from edema, an orange-peel appearance of the breast is associated with cancer.
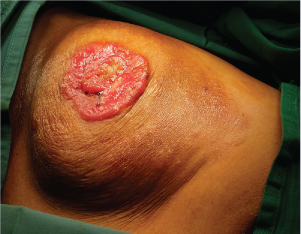
Redness and flaking of the nipple may be seen early in Paget disease and then disappear. However, further assessment is needed as this does not mean the disease is gone. Tingling, itching, increased sensitivity, burning, discharge, and pain in the nipple are late signs of Paget disease. It may occur in both breasts, but is rare.
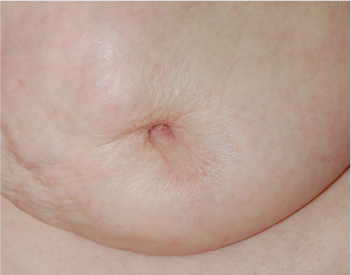
NIPPLE INVERSION FROM BREAST CANCER
Nipple inversion may suggest malignancy.
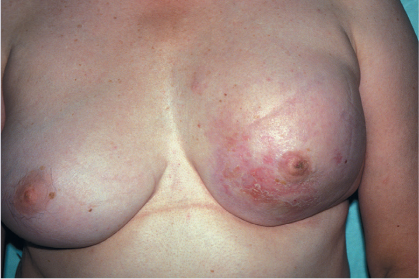
Reddened, painful area on breast warm to palpation.
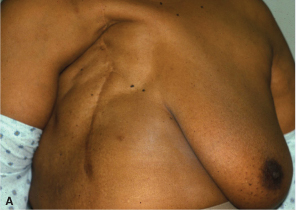
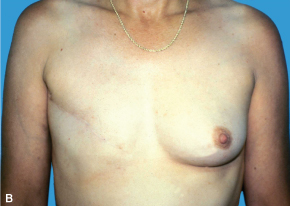
(A) Radical mastectomy. (B) Modified radical mastectomy.
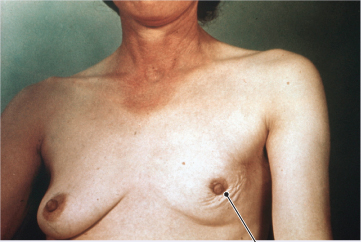
CARCINOMA OF THE BREAST (NOTE BULGING AND SKIN CHANGES)
Photo credits: Retracted breast tissue, carcinoma of the breast, and gynecomastia, reprinted with permission from Jensen, S. (2019). Nursing health assessment: A best practice approach (3rd ed., Table 19-4 (part)). Wolters Kluwer; nipple inversion from breast cancer, reprinted with permission from Harris, J. R., Lippman, M. E., Morrow, M., & Osborne, C. K. (2014). Diseases of the breast (5th ed.). Lippincott Williams & Wilkins; mastitis, reprinted with permission from Hatfield, N. T., & Kincheloe, C. (2017). Introductory maternity and pediatric nursing (4th ed.). Wolters Kluwer; mastectomy, reprinted with permission from Berek, J. S., Hacker, N. F. (2014). Berek and Hacker’s gynecologic oncology (6th ed.). Lippincott, Williams & Wilkins.Although rare, men can have breast cancer, which may not be caught until the late stages, because many in society are unaware of its occurrence in men (American Cancer Society [ACS], 2020a).
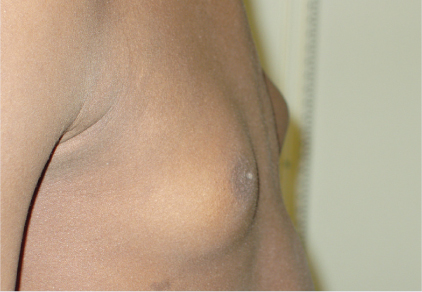
Inspect and palpate breast with client seated, arms at sides. Palpate lymph nodes. No swelling, ulcerations, or nodules should be noted. Flat disc of undeveloped breast tissue under nipple is normally palpated. Soft fatty tissue enlargement seen in obesity. Gynecomastia (Fig. 16-8) and a smooth, firm movable disc of glandular tissue may be seen in one breast during puberty for a short time and may be seen in hormonal imbalances (disease or medication induced) and drug abuse. Irregular, hard nodules are seen in malignancy.
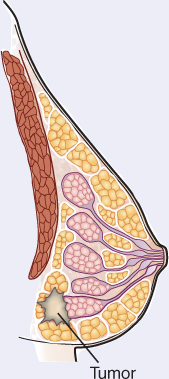
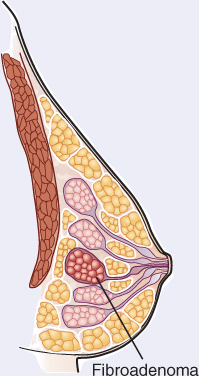
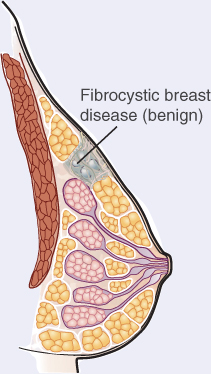
Whereas some abnormalities of the breast are readily apparent, such as peau d’orange and Paget disease, some breast internal changes are detected only by palpation and mammography. The following illustrations represent breast abnormalities characteristic of tumors, fibroadenomas, and benign disease (fibrocystic breasts).
These are irregular, firm, hard, undefined masses that may be fixed or mobile. They are not usually tender and usually occur after age 50.
These lesions are lobular, ovoid, or round. They are firm, well defined, seldom tender, and usually singular and mobile. They occur more commonly between puberty and menopause.
Also called fibrocystic breast disease, benign breast disease is marked by round, elastic, defined, tender, and mobile cysts. The condition is most common from age 30 to menopause, after which it decreases.
Age of menarche? Asymmetrical breast growth? Girls prior to puberty: pain or discomfort? Boys during adolescence: abnormal increase in size?
See normal breast development in Chapter 23, Table 23-1, which varies with age. Adolescent breast development is usually seen between the ages of 10 and 13 years and takes about 3 years for full development.
Breasts pendulous, atrophied, and less firm owing to a decrease in estrogen levels.
May have smaller, flatter nipples that are less erectile on stimulation. Nipples may retract, but will evert with gentle pressure.
Genetic variation: About 5% to 10% of breast cancer cases are thought to be hereditary. BRCA1 and BRCA2 genes are the most common cause of hereditary breast cancer. In the United States, BRCA mutations are found most often in Jewish women of Ashkenazi (Eastern Europe) origin (Basser Center for BRCA, 2017).
Studies of ethnic variation in developing breast cancer show that White women are slightly more likely to develop breast cancer than Black, Hispanic, and Asian women, but Black women are more likely to develop more aggressive and advanced-stage breast cancer that is diagnosed at a young age ("Race/ethnicity," 2020). Black women are also more likely to die from breast cancer. Differences may be due to varying access to medical care, diet differences, and other lifestyle issues.