Actinic (Solar) Keratosis on the Cheek
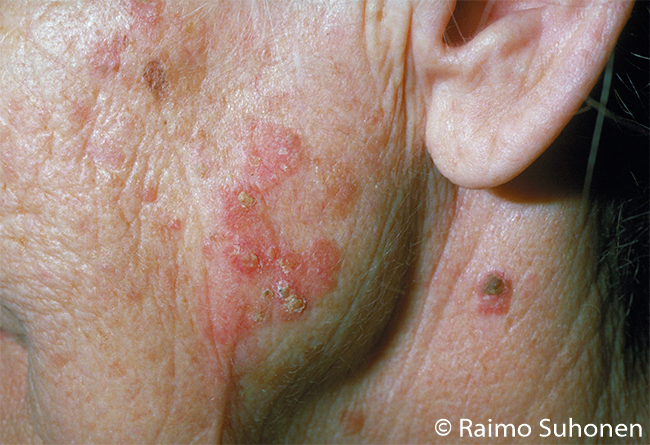
Actinic (solar) keratosis on the cheek. A relatively extensive solar keratosis (actinic keratosis). Bowen's disease should be considered in differential diagnosis.
Picture and text: Raimo Suhonen
Primary/Secondary Keywords
- Dermatology
- keratosis actinica
- actinic keratosis
- solar kerotosis
- Mb Bowen
- Bowen disease
- cheek
- face