Insulin is secreted by the 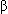 cells in response to elevated blood glucose, certain amino acids, ketones, fatty acids, cortisol, growth hormone, glucagon, gastrin, secretin, cholecystokinin, gastric inhibitory peptide, estrogen, and progesterone. Because of normal feedback mechanisms, high insulin levels inhibit secretion of insulin. Elevated blood levels of somatostatin, epinephrine, and norepinephrine also inhibit insulin secretion.
cells in response to elevated blood glucose, certain amino acids, ketones, fatty acids, cortisol, growth hormone, glucagon, gastrin, secretin, cholecystokinin, gastric inhibitory peptide, estrogen, and progesterone. Because of normal feedback mechanisms, high insulin levels inhibit secretion of insulin. Elevated blood levels of somatostatin, epinephrine, and norepinephrine also inhibit insulin secretion.
Abnormally elevated serum insulin levels are seen with insulin- and proinsulin-secreting tumors (insulinomas), with reactive hypoglycemia in developing diabetes mellitus, and with excessive administration of exogenous insulin.
A blood glucose level is usually obtained with the serum insulin determination. Serum insulin levels may also be measured when glucose tolerance tests are performed.
Nursing Care Before the Procedure
Client preparation is the same as that for the related blood glucose test (e.g., fasting blood glucose, glucose tolerance test) with which the serum insulin determination is performed.
The general procedure is the same as that for the related blood glucose test. Blood samples for serum insulin determinations are obtained in red-topped tubes and then packed in ice. The samples should be handled gently to avoid hemolysis and sent immediately to the laboratory.
Nursing Care After the Procedure
Care and assessment after the procedure are the same as for the related blood glucose test.
- Assess the client for signs of hypoglycemia, which may occur in response to fasting or excessive blood glucose load.
- Resume foods and any medications withheld before the test.
- Abnormal values: Note and report decreased or increased levels and relation to type I or II diabetes mellitus, respectively, and response to glucose intake.
- Critical values: Notify the physician at once if fasting level is greater than 30 U/mL. Prepare client for glucose administration.
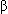 cells in response to elevated blood glucose, certain amino acids, ketones, fatty acids, cortisol, growth hormone, glucagon, gastrin, secretin, cholecystokinin, gastric inhibitory peptide, estrogen, and progesterone. Because of normal feedback mechanisms, high insulin levels inhibit secretion of insulin. Elevated blood levels of somatostatin, epinephrine, and norepinephrine also inhibit insulin secretion.
cells in response to elevated blood glucose, certain amino acids, ketones, fatty acids, cortisol, growth hormone, glucagon, gastrin, secretin, cholecystokinin, gastric inhibitory peptide, estrogen, and progesterone. Because of normal feedback mechanisms, high insulin levels inhibit secretion of insulin. Elevated blood levels of somatostatin, epinephrine, and norepinephrine also inhibit insulin secretion.