AUTHORS: Helen B. Gomez Slagle, MD and Anthony Sciscione, DO



DefinitionCervicitis is an inflammation of the uterine cervix, primarily affecting the columnar epithelial cells of the endocervical glands. Acute cervicitis results from direct infection of the cervix secondary to a uterine or vaginal infection-most commonly chlamydia or gonorrhea-whereas chronic cervicitis is due to an exposure to a local irritant.
SynonymsEndocervicitis
Ectocervicitis
Mucopurulent cervicitis
| ICD-10CM CODES | | N72 | Inflammatory disease of cervix uteri | | A54.03 | Gonococcal cervicitis, unspecified | | A74.89 | Other chlamydial diseases | | A60.03 | Herpesviral cervicitis | | O86.11 | Cervicitis following delivery |
|
Epidemiology & DemographicsThe published prevalence of cervicitis varies greatly, ranging from 8% to as high as 40% of women attending sexually transmitted disease (STD) clinics. Cervicitis is most common in women aged 15 to 24, but it can occur in any sexually active woman. Women who have had sex without condoms or sex with multiple partners are at increased risk of developing cervicitis as well as other STDs.
Physical Findings & Clinical Presentation
- Cervicitis is usually asymptomatic or associated with mild symptoms. Patients may complain of copious purulent or mucopurulent vaginal discharge, pelvic pain, postcoital or intermenstrual bleeding, vulvovaginal irritation, or dyspareunia.
- The CDC emphasizes that the two diagnostic signs of cervicitis are either mucopurulent discharge or sustained cervical bleeding with gentle trauma. On physical exam, the cervix can be erythematous and tender on palpation. The cervix may also bleed easily when obtaining cultures or a Pap smear. Yellow discharge will be seen on a Q-tip inserted into the cervix.
Infectious Etiology
- Chlamydia trachomatis
- Neisseria gonorrhoeae
- Trichomonas vaginalis
- Herpes simplex
- Human papillomavirus
- M. genitalium
- Bacterial vaginosis

The diagnosis of acute cervicitis is clinical and based upon the presence of purulent or mucopurulent cervical exudate (Fig. E1) and/or cervical friability-bleeding induced by gently touching the area with a swab.
Figure E1 Mucopurulent cervicitis.
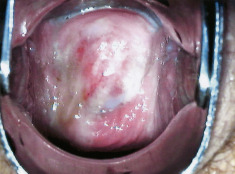
This may be a feature of infection with C. trachomatis or N. gonorrhoeae. The cervix, however, can look normal.
From Magowan BA: Clinical obstetrics and gynaecology, ed 4, Philadelphia, 2019, Elsevier.
Differential Diagnosis
- Carcinoma of the cervix
- Cervical erosion (from tampons or other intravaginal devices)
- Cervical metaplasia
- Cervical ectropion
- Cervical and vaginal irritation due to chemicals or hormonal imbalance
WorkupIf cervicitis is suspected, testing for infectious causes should be performed, and pelvic inflammatory disease (PID) should be excluded.
Laboratory Tests
- A finding of leucorrhea (>10 WBC per high-power field on microscopic examination of vaginal fluid) has been associated with chlamydial and gonococcal infection of the cervix.
- Nucleic acid amplification tests (NAAT) should be used for diagnosing C. trachomatis and N. gonorrhoeae in women with cervicitis; this testing can be performed on vaginal, cervical, or urinary samples.
- Use a wet mount to look for evidence of bacterial vaginitis (BV) and trichomonads, but because the sensitivity of microscopy to detect T. vaginalis is relatively low (∼50%), symptomatic women with cervicitis and negative microscopy for BV and trichomonads should receive further testing with NAAT or culture if there is concern for resistant infection.
- HIV testing is recommended in all patients with suspected cervicitis.
- Although HSV-2 infection has been associated with cervicitis, the utility of specific testing (i.e., culture or serologic testing) for HSV-2 in this setting is not recommended unless there are clinical findings suggestive of herpes infection.
