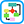
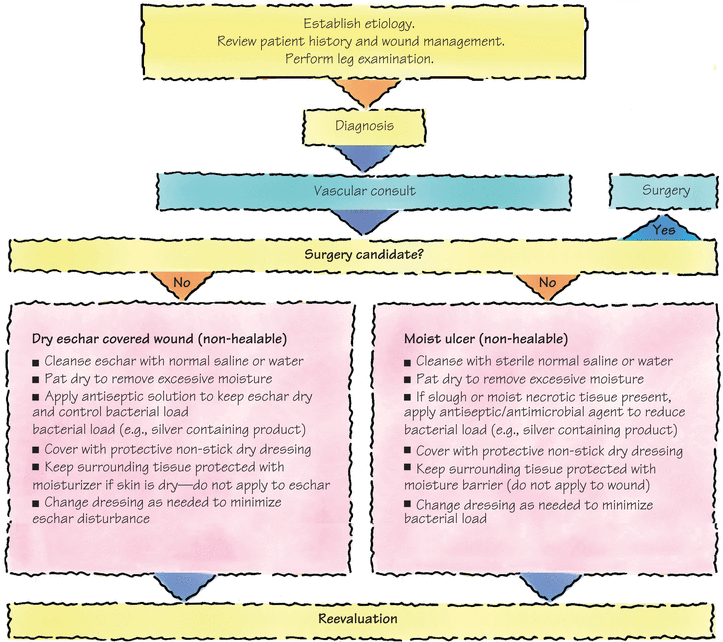
Effective treatment of a vascular ulcer involves caring for the wound as well as managing the underlying vascular disease. The goals and treatment recommendations vary depending on the type of ulcer.
| Type of ulcer | Treatment goals | Therapies and procedures | Wound care |
|---|
| Venous | - Control edema
- Manage underlying venous disease
- Provide appropriate wound care
| - Limb elevation to allow gravity to drain fluid from the limb
- Compression bandages, layered compression bandages, elastic bandages, compression pumps, compression stockings, or graduated compression support hosiery to reduce edema
- Bandaging and wrapping (paste wrap such as Unna's boot) may be used to provide compression, protection, and a moist environment for healing
| - Apply dressings to promote moist wound healing, growth of granulation tissue, and reepithelialization.
- Apply growth factors to the wound bed, as ordered, to improve healing rate.
- Consider advanced wound healing technologies such as cellular tissue products (CTPS) for a venous ulcer that fails to heal within 4 weeks of treatment.
| | Arterial | - Reestablish arterial flow
- Provide appropriate wound care and wound protection
| - Arterial bypass to restore arterial flow
- Angioplasty (with possible stent insertion) to treat arterial stenosis
| - Keep the wound dry and protected from pressure or trauma.
- As ordered, apply an antiseptic or antimicrobial agent and then place small gauze pads between the toes. Change the pads daily to keep toe ulcers dry.
- Never soak arterial ulcers.
- If revascularization succeeds, change the type of dressing to keep moist tissue moist and dry tissue dry.
| | Lymphatic | - Reduce edema
- Prevent infection
- Provide appropriate wound care
| - Limb elevation and compression pump therapy to reduce edema
- Comprehensive decongestive therapy (a form of massage) to reduce edema and improve circulation
| - Follow guidelines for venous ulcer care.
- Choose dressings that can manage large fluid loads while protecting the surrounding skin, such as foams and other absorbent dressings.
- Negative pressure wound therapy may be a good alternative to dressings for copious fluid leakage.
|
|
Take note Documenting compression bandage application |
Best dressed Dressings for vascular ulcers| Dressing | | Indications and contraindications |
|---|
| Venous ulcers | Arterial ulcers | Lymphatic ulcers |
|---|
| Alginate/hydrofiber | - Use to manage copious drainage.
| - Use to manage copious drainage.
| - Use to manage copious drainage.
| | Foam | - Use to protect the ulcer.
- Use for absorption underneath a compression dressing.
| - Use to protect the ulcer.
- Use with dry gangrene.
- Use for a moist, revascularized ulcer.
| - Use to protect the ulcer.
- Use to absorb drainage.
| | Hydrocolloid | - Use to promote granulation.
- Use to manage pain.
- Don't use when copious drainage is present.
| - Use for autolytic debridement.
- Use for primary dressing after revascularization.
- Don't use on ischemic tissue.
- Don't use when infection or cellulitis is present.
| - Use to protect the skin.
- Use to promote epithelialization.
- Don't use when copious drainage is present.
- Don't use when cellulitis is present.
| | Hydrogel | - Don't use when copious drainage is present.
| - Use to maintain a moist wound bed.
- Use for autolytic debridement.
| - Use to manage pain.
- Use for autolytic debridement.
| | Transparent film | | - Use only after the ulcer has almost completely healed.
| - Use to protect fragile skin.
|
|
|