AUTHORS: Lakshmi Ravindra, MD and Ross W. Hilliard, MD, FACP
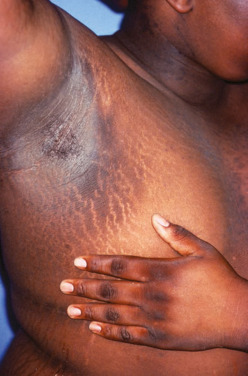
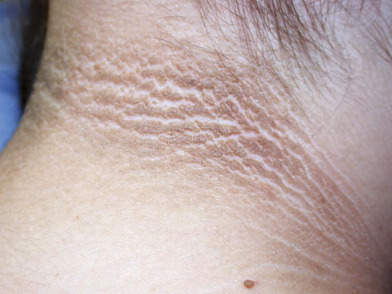
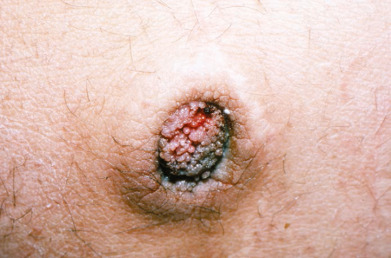
Acanthosis nigricans (AN) is a condition described as dark, velvety, thickened skin in a symmetric distribution more commonly located in intertriginous areas including the axillary (Fig. E1), neck (Fig. E2), and groin regions. It is generally associated with insulin resistance due to diabetes and/or obesity; however, it can less frequently occur in the setting of an underlying malignancy (Fig. E3), medications, or congenital syndromes.1
Figure E1 Acanthosis nigricans in the axillary.
From Micheletti RG et al: Andrews’ diseases of the skin, clinical atlas, ed 2, Philadelphia, 2023, Elsevier.
Overall, reported prevalence varies significantly from study to study, and evaluations of prevalence between ethnicities are limited. From the data available, AN appears to be more common in Black Americans, Native Americans, and Hispanic Americans in the United States as compared to White or Asian Americans in individuals of all ages.2
Individuals with AN are generally asymptomatic but may experience pruritus. Physical features include symmetric, thickened areas of skin that are hyperpigmented in nature and with a velvety texture. Initially, the areas of skin affected have a grey-brown/black pigmentation and are dry and rough. The most commonly affected areas include the axillae, groin, back and sides of the neck, and popliteal areas, also known as the intertriginous areas. In extensive cases of AN, the lips, conjunctiva, areola, and buccal mucosa may also be involved.1,2
AN is a result of high insulin levels leading to both direct and indirect activation of insulin-like growth factor (IGF) receptors on fibroblasts and keratinocytes, thus stimulating growth and proliferation that results in AN. Tyrosine kinase receptors like epidermal growth factor receptor (EGFR) and fibroblast growth factor receptor (FGFR) are also thought to be mediators. While hyperinsulinemia is thought to promote AN, it is also hypothesized that friction and perspiration contribute given the location of the typical areas of AN. Different classifications of AN have been proposed, though most classifications share the categories of benign versus malignant/paraneoplastic.1,4,5